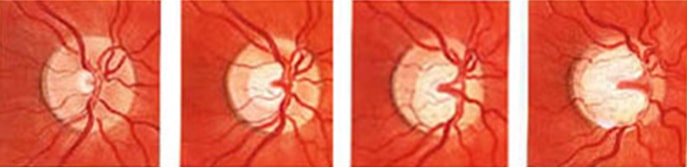
GLAUCOMA CAUSES
Glaucoma is an increase in intraocular pressure, creating a gradual but irreversible reduction of the visual field and of the visual function due to a permanent damage to the optic nerve. A treatment, whichever it may be, can only stabilize the ocular function but under no circumstance can it allow the recovery of an impaired visual function. One should therefore not wait for a decrease in visual acuity to consult a specialist. The origin of glaucoma is usually unknown, but there is nevertheless a strong family heredity. Some local or general treatments, especially corticosteroid therapy, can promote or accelerate the onset of glaucoma in predisposed patients.
GLAUCOMA TREATMENT
A surgical intervention is needed when, despite medical treatment, the tension is too high and/ or the visual field is inevitably deteriorating. The current trend is not to delay the surgery too much, as it is all the more effective when the number of eye drops required to maintain intraocular pressure control is low. Using modern techniques of ocular microsurgery, the procedure consists in facilitating the evacuation of aqueous humour through the creation of an internal bypass beneath the conjunctiva, which often results in the appearance of an outgrowth called ‘bleb’ located below the eyelid. The bypass can be partial (deep sclerectomy) or total (trabeculectomy).
The length of stay at the clinic will be approximately two hours. Patients should arrive about one hour prior to surgery, which will take place under local anaesthesia. The average length of the procedure is around fifteen minutes, with a 30 to 40 minute preparation in the operating room. A snack is served after the intervention, immediately before departure. A protective shell is placed on the operated eye until the day after the intervention, and is replaced by a pair of glasses – no matter which type – whose role is to protect the eye from a possible shock the following days. Local treatments last several weeks and consist in the instillation of eye drops, and sometimes in the application of an ointment.
In a few particular cases, hospitalization may be useful or necessary. Its duration will be determined accurately in an “à la carte” fashion at the time of the preoperative office visit. The decision will take into account medical requirements (e.g. anticoagulant treatment), personal preferences, the family environment, the place of housing, etc.
The procedure can in no way claim to improve vision, and can only stabilize the visual function in order to prevent further degradation. However, it has an excellent success rate.
GLAUCOMA COMPLICATIONS
Zero risk surgery unfortunately does not exist, including glaucoma surgery. Exceptional and unforeseen issues can thus be observed at the time of surgery or during the postoperative period. In the short-term, vision can drop significantly during the first postoperative weeks due to intraocular bleeding or to a bypass running too well and excessively lowering the intraocular pressure. These two phenomena usually spontaneously subside and vision returns to its pre-surgery level. However, in some cases, the persistence of an abnormally low tension may necessitate a reoperation. Rare but serious, postoperative infections (1/1000) are characterized by a painful eye as well as abundant secretions. They require an urgent consultation and an aggressive treatment.
Other complications are less severe. They can for instance be an insufficiently tight scar, a partial collapse of the upper eyelid, a hematoma in the white of the eye or eyelid, or a certain degree of eye irritation caused by postoperative hypotonia and/ or sutures – which usually spontaneously reabsorb themselves in a fortnight.
Generally, anti-glaucomatous interventions promote the onset or worsening of a cataract in the medium-term, which is the source of a potential decreased visual acuity. In that case, a cataract surgery will again restore the visual function at the time of glaucoma surgery.
In the long-term, filtration bubbles that emerged after surgery – which usually manifest themselves through the appearance of a lump under the eyelid – must be regularly inspected during consultations with your doctor in order to prevent any secondary infection linked to their deterioration.
In 70-80% of cases, anti-glaucomatous interventions enable patients to stop using any anti-glaucoma eye drops. More rarely, it will be necessary to undertake a maintenance treatment associated with the surgery, enabling both the completion of the balance of glaucoma and the preservation of the visual function in a long-term period.
GLAUCOMA CONCLUSION
Glaucoma surgery has nowadays proven its maturity. Though it may, like any other surgical procedure, encounter problems – such as inadequate healing, risk of infection, or other unpredictable hazards including the need for a reoperation – it nonetheless generates overall a great satisfaction among surgical patients.
GLAUCOMA: IMAGES
Image : irreversible damage to the optic nerve